samedi 31 octobre 2015
vendredi 30 octobre 2015
Relative risk of cancer, refined nutrients and specific foods
Sugar increases pancreatic cancer risk.
"During a mean follow-up of 7.2 y, we identified 131 incident cases of pancreatic cancer. The consumption of added sugar, soft drinks, and sweetened fruit soups or stewed fruit was positively associated with the risk of pancreatic cancer. The multivariate hazard ratios for the highest compared with the lowest consumption categories were 1.69 (95% CI: 0.99, 2.89; P for trend = 0.06) for sugar, 1.93 (1.18, 3.14; P for trend = 0.02) for soft drinks, and 1.51 (0.97, 2.36; Pfor trend = 0.05) for sweetened fruit soups or stewed fruit."http://ajcn.nutrition.org/content/84/5/1171/T2.expansion.html
http://ajcn.nutrition.org/content/84/5/1171.full
Fructose sucrose and GL increase the risk of colorectal cancer in men
http://cebp.aacrjournals.org/content/14/1/138/T2.expansion.html
http://cebp.aacrjournals.org/content/14/1/138.long
Meat and colorectal cancer
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4420687/figure/F1/http://www.ncbi.nlm.nih.gov/pubmed/25751512
 |
| Viande rouge neutre pour le risque de cancer colorectal |
 |
| Essentiellement les saucisses |
Absolute Risk of breast cancer
According to the current report, the risk that a woman will be diagnosed with breast cancer during the next 10 years, starting at the following ages, is as follows:
- Age 30 . . . . . . 0.44 percent (or 1 in 227)
- Age 40 . . . . . . 1.47 percent (or 1 in 68)
- Age 50 . . . . . . 2.38 percent (or 1 in 42)
- Age 60 . . . . . . 3.56 percent (or 1 in 28)
- Age 70 . . . . . . 3.82 percent (or 1 in 26)
Howlader N, Noone AM, Krapcho M, et. al. (eds). SEER Cancer Statistics Review, 1975–2009 (Vintage 2009 Populations), National Cancer Institute. Bethesda, MD, 2012. Retrieved September 7, 2012.
Low fat versus low sugar
jeudi 29 octobre 2015
Lipids in Acute Myocardial Infarction
Lipid Paradox in Acute Myocardial Infarction—The Association With 30-Day In-Hospital Mortality
Cheng, Kai-Hung MD1,2,3; Chu, Chih-Sheng MD, PhD1,2,3; Lin, Tsung-Hsien MD, PhD1,2,3; Lee, Kun-Tai MD1,2; Sheu, Sheng-Hsiung MD1,2; Lai, Wen-Ter MD1,2
Antioxidants supplements deadly?
- Mejia, Paula. “Antioxidants May Lead to Cancer Spread, Study Says.” Newsweek. 17 October 2015. Available http://www.newsweek.com/antioxidants-may-lead-cancer-spread-study-says-384528
- Piskounova E, Agathocleous M, Murphy MM, et al. Oxidative stress inhibits distant metastasis by human melanoma cells. Nature. 2015.
- Chen AC, Martin AJ, Choy B, et al. A Phase 3 Randomized Trial of Nicotinamide for Skin-Cancer Chemoprevention. The New England journal of medicine. 2015;373(17):1618-1626.
Meat and meat products consumption in France
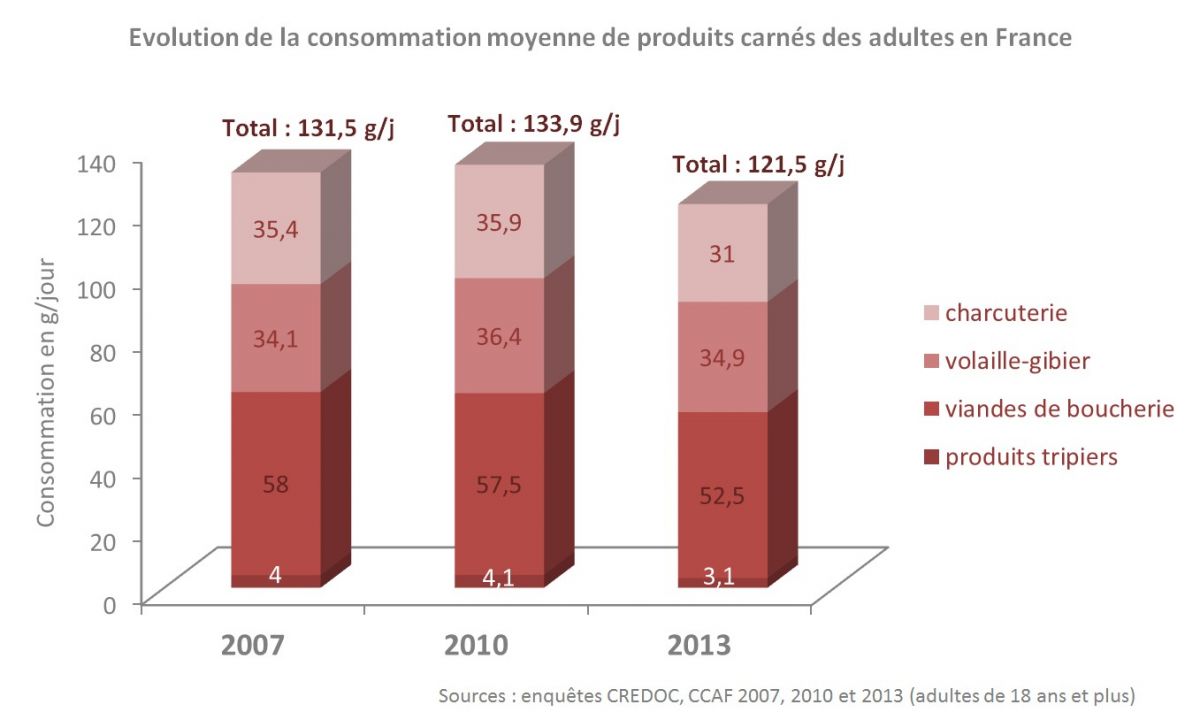 |
| http://www.la-viande.fr/nutrition-sante/consommation-viande-france |
Eat offal especially liver
Egg and D2 in women
mercredi 28 octobre 2015
It is mainly a problem of the irrational mind
Meat or not meat
http://www.slate.com/articles/health_and_science/medical_examiner/2014/01/cancer_risk_from_grilled_meat_is_it_time_to_give_up_smoked_and_fried_foods.html?wpsrc=sh_all_tab_tw_top
http://www.reuters.com/article/2015/10/28/us-health-meat-socialmedia-idUSKCN0SL2UJ20151028
http://www.reuters.com/article/2015/10/28/us-health-meat-california-idUSKCN0SM0B620151028
Sugar calories are not fat calories, actually?
Balsamic vinegar: trendy but full of sugars
17g/100g of sugars
A table spoon is 14,5g of sugar.
A cube is 2,3 g of sugar so 100 g of balsamic vinegar is 7,5 sugar cubes and 100ml id est 1 liter is 75 sugar cubes....
http://ndb.nal.usda.gov/ndb/foods/show/310?manu=&fgcd=
Instead Cider vinegar is only 0,93g sugars /100g, less than half a sugar cube in 100 ml and 4 sugar cubes for a liter...
http://ndb.nal.usda.gov/ndb/foods/show/297?manu=&fgcd=
For red wine vinegar the content of carbs is still less 0,27g/100 ml and 2,7 g/liter. A liitle bit more than a sugar cube...
http://ndb.nal.usda.gov/ndb/foods/show/309?manu=&fgcd=
For your information a regular Cola is 9,94 g of sugar/100ml or 99,4 g of sugar a liter.
But, as a matter of facts there are more sugared Balsamic vinegar: 34 g/ 100g quite a marmelade...
https://www.coopathome.ch/epicerie/aides-culinaires/vinaigre/antica-modena-vinaigre-balsamique/C301008/P3816345/fr?s=rp&rs=202464
mardi 27 octobre 2015
IARC, meat and the economy
This paper is a sum of stupidities...
lundi 26 octobre 2015
FTO sitting and obesity
FTO association and interaction with time spent sitting.
Author information
- 1Department of Epidemiology and Biostatistics, Mel and Enid Zuckerman College of Public Health, University of Arizona, Tucson, AZ, USA.
- 2School of Anthropology, University of Arizona, Tucson, AZ, USA.
Abstract
BACKGROUND/OBJECTIVES:
SUBJECTS/METHODS:
RESULTS:
CONCLUSIONS:
If you eat mainly or a lot of processed meat it is time to shift
Processed meat consumption is associated with an increase risk of cancer. Not completely the same meaning.
But the most important is coming: what is the magnitude of the risk? It is small, rather very small. 11-12 % increase of all cancers risk.
Cutted meat (id est red meat) is associated with a smaller risk so the group of IACR qualified it as uncertain.
1/ Cutted meat is less carcinogenic especially if eaten raw or cooked very gently. Yes the main source of carcinogens in red meat is the result of cooking especially high temperature cooking. That is not news.
Charcoal on meat is carcinogenic as soot for the skin of chimney-sweeps.
2/ What processed meat is less carcinogenic? Obviously processed meat freshly prepared or dried meat like jerky or raw ham.
3/ Cheeses are probably better with less or no TMAO production in your gut
 |
| http://pubs.acs.org/doi/abs/10.1021/jf505878a |
http://www.thelancet.com/journals/lanonc/article/PIIS1470-2045(15)00444-1/abstract
Processed meat is carcinogenic according to IARC group and red meat is probably carcinogenic. Mechanisms are less clear:
"Substantial supporting mechanistic evidence was available for multiple meat components (NOC, haem iron, and HAA). Consumption of red meat and processed meat by man induces NOC formation in the colon. High red meat consumption (300 or 420 g/day) increased levels of DNA adducts putatively derived from NOC in exfoliated colonocytes or rectal biopsies in two intervention studies.19,20 Few human data, especially from intervention studies, were available for processed meat. Haem iron mediates formation of NOC, and of lipid oxidation products in the digestive tract of human beings and rodents. Haem iron effects can be experimentally suppressed by calcium, supporting its contribution to carcinogenic mechanisms. Meat heated at a high temperature contains HAA. HAA are genotoxic, and the extent of conversion of HAA to genotoxic metabolites is greater in man than in rodents. Meat smoked or cooked over a heated surface or open flame contains PAH. These chemicals cause DNA damage, but little direct evidence exists that this occurs following meat consumption."
So if you have to choose eat preferably cut meat, raw (tartare) or gently cooked... Avoid products with processed meat. Indeed fresh saucisse or saucisson or jerky or raw dried ham are OK but other products are highly processed...
Evil in the details as usual.
Acrylamide
http://www.sciencedirect.com/science/article/pii/B9780123849472000052
Le titre du pire article sur le gras en français vient d'être décerné!
Faire de la pub pour les acides gras trans en 2012 est une faute.
Tout le reste est à l'avenant du relativisme scientifique.
Low carb diets are doing better on weight loss and CVD risk factors.
Still a great difference between races:
| This is not negligible and side effects are few. |
Stone after stone the destruction of the low fat myth which fueled so many mistakes and so much benefit for agro-industry.
The results of this study on conventional biomarkers of CVD are amazing.
Another time looking at those results marker by marker is totally irrational. The risk is far better appreciated by the combination of factors.
Example: LDL
Low fat works better on LDL BUT we don't know if the LDL particles are the same on low fat diets and low carb diets... And several studies showed that LDL particles profile is more atherogenic on high carb diet and very atherogenic if the carbs do have a high GI.
In the same comparison low fat diets DO NOT improve substantially HDL contrary to low carb diets and we know that the ratio between HDL/LDL particles is a potent risk factor. In the same perspective of global lipid evaluation low carb drastically decrease TG. TG is an independent risk factor of atheroma through chylomicron remnants and VLDL especially in the postprandial period.
My point is that low carb diets moderately decrease all cholesterol containing particles and improve the number and/or size of the HDL particles so the non HDL cholesterol particles decrease. These non HDL cholesterol particles are the major biomarker of atheroma in the lipid heart hypothesis. In summary low carb diets impact all the biomarkers of atheroma instead of low fat diets which are only decreasing LDL cholesterol. Another time total cholesterol is in only some studies poorly correlated with CVD and should not have been mentioned in this comparison.
But lipids are not by far the only biomarkers of atheroma.
Low carb diets which are very efficient on weight (-12 vs -6,5 %) decrease systolic blood pressure which is the major factor of extracranial atheroma in the supra-aortic trunks where originate 25% of TIA and Stroke.
What about acceptance of those diets?
"The magnitude of carbohydrate and fat restrictions were calculated from the time of lowest daily intake (Table 2), at which time the average carbohydrate intake was 145 g/day lower in the LoCHO vs. LoFAT group. The LoFAT group averaged lower protein intake (by 36 g/day) and lower fat intake (by 53 g/day) with an average minimum fat intake of 24% of daily energy (95% CI: 21, 27). At the time of the strictest carbohydrate restriction for the LoCHO group, the total caloric intake was not significantly different between groups (1504 vs. 1449 kcal/day for LoCHO and LoFAT, respectively)."
Eventually the data showed that in low carb diets the minimum CHO intake was 29,5 g/d which is easily doable in an everyday life.
In conclusion this study is in keeping with strong observational nutritional data: Switzerland and France which have the most important consumption of sat fat in Europe (around 15% of TEI) have the lowest rate of CVD. And their sat fats come primarily from animal fat with a high % of cheeses.
Should you advice a closely related to follow a ketogenic diet if he or she suffers cancer?
"primum non nocere" but we have to avoid any delay in front of new chances to cure!
1/ During chemo it is well backed that fasting and enhanced nutrition improve the efficacy and tolerance (stem cells recovery) of chemo. The last study is a RCT!
http://www.ncbi.nlm.nih.gov/pubmed/26438237
http://www.biomedcentral.com/1471-2407/15/652 free full text
http://stm.sciencemag.org/content/4/124/124ra27
2/ Ketogenic diet is on the rise. It is a lie to assert that it can cure cancer. It is very difficult without advice to implement a keto diet when you are the kind of people who eats the standard western diet. Counselling is very difficult to find in Europe.
There are good indications of keto diet in cancer like brain tumors. But another time don't embark alone in keto diet especially if you have cancer.
- caloric restriction is key
- low carb diet is mandatory only one raw juicy fruit at each meal
- you need high fat diet to survive so eat it! Pork, lamb, bone marrow broth, butter, cream, cheeses with long fermentation and affinage in order to avoid any residual lactose, nuts macadamia Brazil nuts and groundnuts.
- eat your protein too, you cannot do it without meat or fish and obviously with eggs.
- no carbs but a lot of veggies, kale, sauerkraut, tomatoes, salads, celery, broccoli no tubers.
You can improve your metabolism and starve your cancer cells.
dimanche 25 octobre 2015
samedi 24 octobre 2015
vendredi 23 octobre 2015
The début of biotech
High fat diet in mice and glucose tolerance: not a reliable model for humans
This title recalled me how reporting science is difficult...
1/ figures 3,4 and 5 of the paper are not available...
2/ reference: http://onlinelibrary.wiley.com/doi/10.1111/bph.13343/abstract
3/ The HFD in mice is a model to study GLUCOSE intolerance!
http://diabetes.diabetesjournals.org/content/53/suppl_3/S215.full
4/it is not a matter of specific fatty acids except for W3 PUFA which are not associated with glucose intolerance:
"Also, in our own study, we were not able to detect significant correlations between the saturation level of free fatty acids and insulin action as estimated from whole-body glucose disposal after an insulin challenge (Figure 2)."
http://onlinelibrary.wiley.com/doi/10.1038/oby.2007.608/full
As usual those exp studies on rodents should be reported with extreme caution about any translational knowledge applicable to humans. issues about carbs and fats are complex and extremely controversial so a more balanced approach should be to report also other studies by instance this one:
"Results: Higher TC, higher HDL-C, and lower triglycerides were associated with higher age 70 cognitive scores in most cognitive domains. These relationships were no longer significant after covarying for childhood IQ, with the exception a markedly attenuated association between TC and processing speed, and triglycerides and age 70 IQ. In the fully adjusted model, all conventionally significant (p < 0.05) effects were removed. Childhood IQ predicted statin use in old age. Statin users had lower g, processing speed, and verbal ability scores at age 70 years after covarying for childhood IQ, but significance was lost after adjusting for TC levels.
Conclusions: These results suggest that serum cholesterol and cognitive function are associated in older age via the lifelong stable trait of intelligence. Potential mechanisms, including lifestyle factors, are discussed."
http://dysnutrition.blogspot.fr/2015/10/cholesterol-and-cognitive-function.html
The surge of nut oils in EU
 |
| The message that consumers send to manufacturers is simple: in EU taste is key! |
Among fatty acid-rich vegetable oil coconut is special. Without big brand it is succeeding to be a trendy in UE and US despite the conventional warnings about sat fats.
http://www.foodnavigator.com/Market-Trends/Coconut-oils-and-spreads-becoming-popular-in-Europe
http://www.foodnavigator.com/Science/Coconut-oil-could-combat-tooth-decay
jeudi 22 octobre 2015
Toujours le sucre mais vous le savez c'est écrit sur presque tous les produits...
Sur le sucre ajouté cette naiveté est partagée par nos concitoyens qui ne lisent pas les ingrédients contenus dans les produits qu'ils achètent car ils sauraient que l'inondation à petit débit est un fait. Pas plus qu'ils ne lisent les recommandations pour les médicaments ou bien qu'ils ne lisent le programme des hommes politiques pour lesquels ils votent...
http://www.bilan.ch/catherine-nivez/sucre-verite-acide
Après il y a le mythe naturaliste:
"Ce sucre artificiel (qui n’a rien à voir avec le fructose des fruits)"
Si, si le fructose du maïs des fruits ou de la synthèse chimique sont les mêmes molécules...
"Les Etats-Unis ont inventé le "fructose de maïs" pour exploiter au maximum leur stock de maïs. C’était économiquement intelligent."
Non, non pas intelligent but heavily subsidised. Like in Europe and singulièrement en France ou le maïs demande une grande quantité d'eau et de pesticides.
mercredi 21 octobre 2015
Cholesterol and cognitive function
International Psychogeriatrics (2015), 27: 439-453
Copyright © International Psychogeriatric Association 2014
doi: 10.1017/S1041610214001197 Publié en ligne : juil. 2014
Serum cholesterol and cognitive functions: the Lothian Birth Cohort 1936
- Article author query
- corley j [PubMed] [Google Scholar]
- starr jm [PubMed] [Google Scholar]
- deary ij [PubMed] [Google Scholar]
Janie Corleya1, John M. Starra2a3 and Ian J. Dearya1a2 c1
a1 Department of Psychology, University of Edinburgh, 7 George Square, Edinburgh EH8 9JZ, UK
a2 Centre for Cognitive Ageing and Cognitive Epidemiology, University of Edinburgh, 7 George Square, Edinburgh EH8 9JZ, UK
a3 Royal Victoria Building, Western General Hospital, Porterfield Road, Edinburgh EH4 2XU, UK
ABSTRACT
Background: We examined the associations between serum cholesterol measures, statin use, and cognitive function measured in childhood and in old age. The possibility that lifelong (trait) cognitive ability accounts for any cross-sectional associations between cholesterol and cognitive performance in older age, seen in observational studies, has not been tested to date.
Methods: Participants were 1,043 men and women from the Lothian Birth Cohort 1936 Study, most of whom had participated in a nationwide IQ-type test in childhood (Scottish Mental Survey of 1947), and were followed up at about age 70 years. Serum cholesterol measures included total cholesterol (TC), high-density lipoprotein cholesterol (HDL-C), triglycerides, and cholesterol:HDL cholesterol ratio. Cognitive outcome measures were age 70 IQ (using the same test as at age 11 years), general cognitive ability (g), processing speed, memory, and verbal ability.
Results: Higher TC, higher HDL-C, and lower triglycerides were associated with higher age 70 cognitive scores in most cognitive domains. These relationships were no longer significant after covarying for childhood IQ, with the exception a markedly attenuated association between TC and processing speed, and triglycerides and age 70 IQ. In the fully adjusted model, all conventionally significant (p < 0.05) effects were removed. Childhood IQ predicted statin use in old age. Statin users had lower g, processing speed, and verbal ability scores at age 70 years after covarying for childhood IQ, but significance was lost after adjusting for TC levels.
Conclusions: These results suggest that serum cholesterol and cognitive function are associated in older age via the lifelong stable trait of intelligence. Potential mechanisms, including lifestyle factors, are discussed.
(Received March 06 2014)
(Reviewed April 27 2014)
(Revised May 13 2014)
(Accepted May 28 2014)
(Online publication July 15 2014)
Correspondence
c1Correspondence should be addressed to: Ian J. Deary, Department of Psychology, Centre for Cognitive Ageing and Cognitive Epidemiology, University of Edinburgh, 7 George Square, Edinburgh EH8 9JZ, Scotland, UK. Phone: +44-131-650-3452. Email: I.Deary@ed.ac.uk.
mardi 20 octobre 2015
W3/W6 ratio and vegetable saturated fats
lundi 19 octobre 2015
Veganism and sperm quality
"Lacto-ovo vegetarians had significantly lower sperm concentration (50.7 7.4 M/mL, mean S.E.M.) when compared with nonvegetarians (69.6 3.2 M/mL). Furthermore, total motility was lower in the lacto-ovo group (33.2 3.8% versus non-vegetarian 58.2 1.0%). Similarly, vegans had lower total motility (51.8 13.4%) with a trend towards lower sperm concentration (51.0 13.1 M/mL). Interestingly, hyperactive motility was lowest in the vegan group. The percent strict normal sperm morphology in all groups were within normal range. There were no differences in the remaining parameters: rapid progression, chromatin integrity and SPA capacitation index. "
http://www.fertstert.org/article/S0015-0282(14)01556-8/fulltext#sec2








